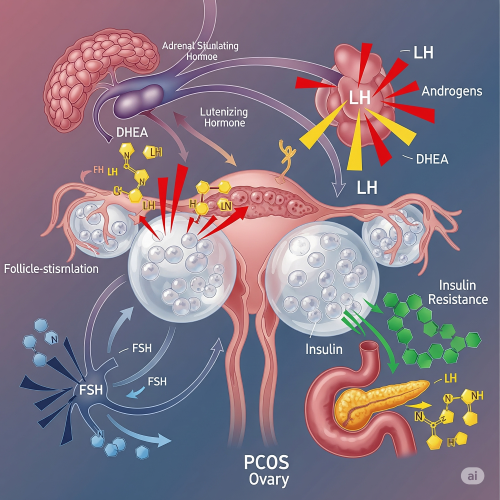
Uncover the complexities of PCOS. Learn about the key factors and potential causes of Polycystic Ovary Syndrome and what you can do about it.
Understanding Polycystic Ovary Syndrome (PCOS)
Polycystic Ovary Syndrome, or PCOS, is a common hormonal disorder that affects women of reproductive age. It’s characterized by a range of symptoms, making diagnosis sometimes challenging. But what causes PCOS? While the exact etiology remains elusive, researchers have identified several contributing factors that increase the likelihood of developing this condition. Understanding these factors can empower women to take proactive steps towards managing their health.
The Role of Genetics
Genetics play a significant role in the development of PCOS. Women with a family history of PCOS, diabetes, or irregular periods are at a higher risk of developing the condition themselves.
– Studies have shown that PCOS tends to cluster in families, suggesting a genetic component.
– Researchers are actively working to identify specific genes that contribute to PCOS susceptibility.
– While no single “PCOS gene” has been identified, it’s likely that multiple genes interact to increase the risk.
Insulin Resistance and PCOS
Insulin resistance is a common finding in women with PCOS and is considered a major contributing factor to the development of the syndrome.
– Insulin is a hormone produced by the pancreas that helps glucose from food get into cells for energy.
– When cells become resistant to insulin, the pancreas produces more insulin to compensate.
– High levels of insulin can trigger the ovaries to produce more androgens, such as testosterone, leading to hormonal imbalances.
– Elevated androgen levels can disrupt ovulation, contribute to the development of cysts on the ovaries, and cause other PCOS symptoms like hirsutism (excess hair growth) and acne.
Hormonal Imbalances in PCOS
Hormonal imbalances are a hallmark of PCOS. These imbalances can affect various aspects of a woman’s health, from her menstrual cycle to her fertility.
Elevated Androgen Levels
As previously mentioned, elevated androgen levels are a key feature of PCOS. These hormones, typically associated with male characteristics, can lead to a variety of symptoms in women.
– Hirsutism: Excessive hair growth on the face, chest, or back.
– Acne: Breakouts that are often resistant to conventional treatments.
– Male-pattern baldness: Thinning hair on the scalp.
– Irregular periods: Disrupted ovulation can lead to infrequent or absent periods.
Luteinizing Hormone (LH) and Follicle-Stimulating Hormone (FSH)
The balance between luteinizing hormone (LH) and follicle-stimulating hormone (FSH) is often disrupted in women with PCOS.
– LH and FSH are hormones that regulate the menstrual cycle and ovulation.
– In PCOS, LH levels may be higher than FSH levels, which can interfere with normal ovulation.
– This hormonal imbalance can contribute to irregular periods and difficulty conceiving.
The Impact of Inflammation
Chronic low-grade inflammation is increasingly recognized as a potential factor in what causes PCOS.
– Studies suggest that women with PCOS have higher levels of inflammatory markers in their blood.
– Inflammation can contribute to insulin resistance and hormonal imbalances, further exacerbating PCOS symptoms.
– Lifestyle factors such as diet, exercise, and stress management can influence inflammation levels.
Environmental and Lifestyle Factors
While genetics and hormones play a significant role, environmental and lifestyle factors can also influence the development and severity of PCOS.
Diet and Exercise
Diet and exercise are crucial for managing insulin resistance and inflammation, both of which are linked to PCOS.
– A diet high in processed foods, sugary drinks, and unhealthy fats can worsen insulin resistance and inflammation.
– Regular physical activity can improve insulin sensitivity, reduce inflammation, and promote weight management.
– A balanced diet rich in whole foods, lean protein, and healthy fats is recommended for women with PCOS.
Stress Management
Chronic stress can disrupt hormone balance and worsen PCOS symptoms.
– When the body is under stress, it releases cortisol, a hormone that can interfere with insulin sensitivity and ovulation.
– Stress management techniques such as yoga, meditation, and deep breathing exercises can help regulate hormone levels.
– Adequate sleep is also essential for managing stress and promoting overall health.
Exposure to Endocrine Disruptors
Exposure to endocrine-disrupting chemicals (EDCs) may play a role in the development of PCOS. EDCs are substances that can interfere with the body’s endocrine system and disrupt hormone balance. [https://www.niehs.nih.gov/health/topics/agents/endocrine/index.cfm]
– EDCs can be found in plastics, pesticides, cosmetics, and other everyday products.
– Some studies have suggested a link between exposure to certain EDCs and an increased risk of PCOS.
– Minimizing exposure to EDCs by choosing natural products, avoiding plastic containers, and eating organic food may be beneficial.
Diagnosing and Managing PCOS
Diagnosing PCOS typically involves a combination of physical examination, blood tests, and ultrasound. Management focuses on addressing individual symptoms and reducing the risk of long-term complications.
Diagnostic Criteria
The Rotterdam criteria are commonly used to diagnose PCOS. The diagnosis requires the presence of at least two of the following three criteria:
1. Irregular periods: Infrequent or absent periods.
2. Hyperandrogenism: Clinical or biochemical signs of elevated androgen levels.
3. Polycystic ovaries: The presence of multiple cysts on the ovaries, as detected by ultrasound.
Treatment Options
Treatment options for PCOS vary depending on the individual’s symptoms and goals.
– Lifestyle modifications: Diet and exercise are often the first line of treatment.
– Medications:
– Birth control pills can regulate periods and reduce androgen levels.
– Metformin can improve insulin sensitivity.
– Spironolactone can block the effects of androgens.
– Fertility treatments: Medications or procedures to help with ovulation.
The Long-Term Health Implications of PCOS
PCOS is not just about irregular periods and acne. It’s a complex condition that can have long-term health implications if left unmanaged.
Increased Risk of Chronic Diseases
Women with PCOS are at an increased risk of developing several chronic diseases.
– Type 2 diabetes: Insulin resistance increases the risk of developing diabetes.
– Cardiovascular disease: PCOS can contribute to high blood pressure, high cholesterol, and other risk factors for heart disease.
– Endometrial cancer: Irregular periods can lead to a thickening of the uterine lining, increasing the risk of endometrial cancer.
Mental Health
PCOS can also affect mental health. Women with PCOS are more likely to experience anxiety, depression, and body image issues.
– Hormonal imbalances and physical symptoms can contribute to mood changes and emotional distress.
– Seeking support from a therapist or counselor can be helpful in managing these mental health challenges.
– Support groups can also provide a sense of community and shared understanding.
Understanding what causes PCOS is the first step in taking control of your health. While the exact cause of PCOS remains unclear, genetics, insulin resistance, hormonal imbalances, inflammation, and environmental factors all play a role. By adopting a healthy lifestyle, managing stress, and working closely with your healthcare provider, you can effectively manage your symptoms and reduce your risk of long-term complications.
Ready to learn more about managing your PCOS symptoms naturally? Explore our other articles for practical tips on diet, exercise, and stress reduction techniques to help you thrive!